From Patient Registration to Reimbursement
Optimizing the Revenue Cycle isn’t just about getting paid
it's about building a future-ready healthcare ecosystem
![[removal.ai]_b1f83ba0-76a5-438f-a17f-46a33fb90dcc-logo-design_ZCBJEF](https://codecredentia.com/wp-content/uploads/2025/06/removal.ai_b1f83ba0-76a5-438f-a17f-46a33fb90dcc-logo-design_ZCBJEF.png)

Optimizing the Revenue Cycle isn’t just about getting paid
it's about building a future-ready healthcare ecosystem

Optimizing the Revenue Cycle isn’t just about getting paid it's about building a future-ready healthcare ecosystem

Optimizing the Revenue Cycle isn’t just about getting paid it's about building a future-ready healthcare ecosystem
In today’s fast-evolving healthcare landscape, mastering the Revenue Cycle is no longer optional it’s essential. From patient scheduling to final reimbursement, understanding each component of the Healthcare Revenue Cycle Management (RCM) process is critical for boosting profitability, compliance, and patient satisfaction.
Whether you’re a healthcare provider, billing expert, or medical coder, this comprehensive guide will walk you through the entire revenue cycle, integrated with 2025 updates and future-proof practices valid through 2030.
The Revenue Cycle encompasses the complete financial process healthcare organizations follow to manage and optimize revenue generated from patient services. It begins the moment a patient schedules an appointment and continues through every stage of care ending only when all payments are collected and accounted for.
A well-managed revenue cycle is essential for operational stability and long-term growth. When executed effectively, it ensures:
Maximum Reimbursement
Accurate coding, proper documentation, and timely claims submission help healthcare providers capture the full value of services rendered.
Regulatory Compliance
Staying up to date with changing healthcare laws, payer policies, and documentation standards minimizes legal and financial risk.
Lower Denial Rates
Proactive eligibility verification, clean claim submissions, and prompt follow-up reduce the likelihood of insurance denials and delays.
Higher Patient Satisfaction
Transparent billing practices, efficient communication, and streamlined payment processes improve the patient experience and build trust.
At its core, the revenue cycle is not just a back-office function it’s a strategic driver of both financial performance and patient care quality.
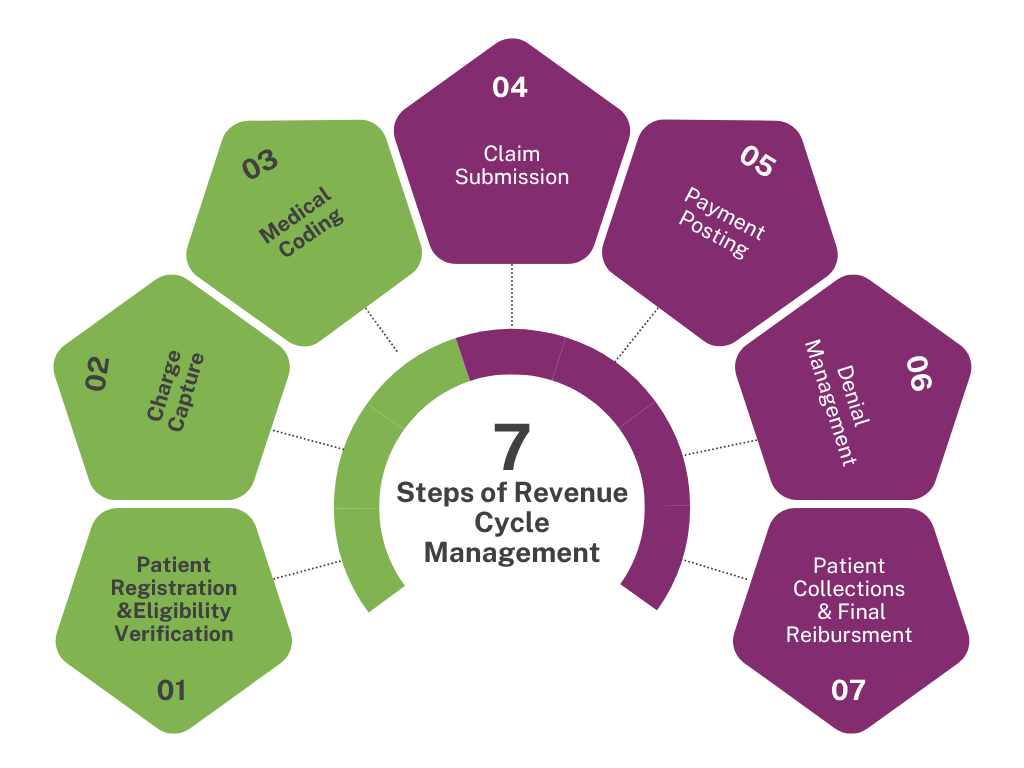
The revenue cycle begins with the most foundational of steps patient registration and insurance eligibility verification. This stage sets the tone for the entire reimbursement process. Mistakes made here often lead to denied or delayed claims downstream.
At the time of scheduling, front-desk or intake staff collect critical information: full name, date of birth, address, insurance provider, policy numbers, and reason for visit. In 2025, this process has been significantly improved by AI-powered real-time eligibility (RTE) checks and integrated Electronic Health Record (EHR) systems that pull payer data instantly.
Under the TEFCA framework, health information exchanges are now more streamlined, enabling accurate and interoperable patient data exchange. Additionally, many clinics use self-registration kiosks and digital intake forms to enhance accuracy and speed.
Once the patient encounter concludes, it’s time to translate the care delivered into charges. This is the charge capture process, where clinical notes are used to assign billable services.
Traditionally manual, this process has evolved in 2025 with Natural Language Processing (NLP) and automated charge capture tools that scan provider documentation for unbilled services. These smart systems not only reduce missed charges but also improve charge lag times, contributing to cleaner claims.
Providers must ensure their documentation is thorough, timely, and properly coded to avoid revenue leakage. Missed or inaccurate charges no matter how small can cumulatively impact the organization’s bottom line.
Medical coding is where documentation is translated into standardized alphanumeric codes that describe diagnoses, procedures, and services rendered. In 2025, the transition toward ICD-11 is underway, and coders are also expected to capture Social Determinants of Health (SDOH) to support value-based care models.
Coders must work meticulously, assigning ICD-11, CPT, and HCPCS codes while adhering to constantly evolving payer policies. Today’s coders are assisted by AI-driven coding platforms that flag inconsistencies, under-coding, or over-coding.
Accurate coding is critical not just for reimbursement but also for data integrity, regulatory reporting, and population health analytics.
With codes in place, it’s time for claim submission a critical milestone in the revenue cycle. A clean claim must include accurate patient data, proper coding, appropriate modifiers, and proof of medical necessity.
In 2025, most claims are submitted electronically through FHIR-based APIs or clearinghouses that interface with payers. These systems now include AI-powered claim scrubbers that automatically detect errors like mismatched diagnosis codes, missing NPI numbers, or expired insurance.
To avoid denials, organizations must implement a robust claims audit process and ensure that every claim is reviewed before submission.
When payers respond to submitted claims, the process of payment posting begins. This involves entering or importing Electronic Remittance Advice (ERA) or Explanation of Benefits (EOB) data into the practice management system.
Accurate posting includes allocating payments, adjustments, write-offs, and patient balances. In modern RCM workflows, Robotic Process Automation (RPA) is widely used to speed up this step, especially in high-volume practices.
Dashboards now allow real-time tracking of key financial metrics such as collection rate, payer performance, and underpayments, helping healthcare finance teams stay in control.
Despite best efforts, not all claims are accepted on first submission. That’s where denial management plays a pivotal role.
Denials must be categorized, analyzed, and resolved systematically. Using predictive analytics, organizations can now proactively identify claims likely to be denied and intervene early. Many healthcare systems employ AI-generated appeal letters to streamline the resubmission process.
The goal is not just to appeal denied claims, but to reduce the occurrence of denials altogether through root cause analysis and continuous process improvement.
The final piece of the revenue cycle puzzle is collecting outstanding balances from patients. With growing out-of-pocket expenses, patient collections are now a major revenue stream.
Modern systems offer self-service digital payment options, including mobile wallets, automated payment plans, and personalized balance segmentation. Clear, transparent billing supported by real-time price estimators builds trust and improves payment rates.
By 2030, it is estimated that more than 80% of patient payments will be made digitally, often without human intervention.
Reduce human error and speed up processing across coding, billing, and posting.

Transparent billing and quick digital payments improve patient retention and revenue.
ICD-11, HIPAA 2025 updates, and federal price transparency mandates are evolving fast.
Platforms like Code Credentia offer real-time courses, certifications, and industry-specific guidance.
The healthcare revenue cycle is no longer just a back office concern it’s a strategic lever for financial health, patient experience, and regulatory compliance. By understanding and optimizing every phase from registration to reimbursement, your organization can not only survive but thrive in the 2025-2030 landscape.
At Code Credentia, we’re committed to helping you navigate this transformation with expert training, updates, and certification support.
Revenue Cycle Management (RCM) is more than just a financial process—it directly impacts the quality of patient care and the sustainability of healthcare organizations. Efficient RCM ensures that healthcare providers can focus on patient care instead of administrative bottlenecks.
A strong revenue cycle allows healthcare providers to:
Reduce claim denials and delays in reimbursement.
Improve cash flow, which is crucial for operational stability.
Enhance patient satisfaction by providing transparent billing and reducing billing errors.
For example, consider a hospital that struggles with delayed claim submissions. Even with high patient volume, the hospital may face cash flow issues because reimbursements are slow. Efficient revenue cycle management would streamline claim submission, follow-ups, and payment posting, resulting in faster revenue collection and better financial health.
Even the best systems face challenges. Highlighting these helps readers understand the importance of strong RCM:
Claim Denials and Delays – Often due to incomplete documentation or incorrect coding.
Patient Financial Responsibility – With high deductibles, patients may struggle to pay, increasing the need for transparent communication.
Regulatory Changes – Constant updates in healthcare regulations require RCM teams to adapt quickly.
Data Management – Maintaining accurate patient data across multiple systems can be tricky.
Modern healthcare organizations increasingly rely on technology to streamline revenue cycle processes:
RCM Software – Helps automate eligibility verification, claim submission, payment posting, and reporting.
Electronic Health Records (EHRs) – Integrate patient data with billing systems for seamless workflows.
Artificial Intelligence – AI tools can predict denials, flag coding errors, and automate repetitive tasks.
Patient Portals – Allow patients to view bills, make payments, and update insurance information.
Example: A hospital using AI-powered RCM software saw a 30% reduction in claim denials within six months.
To maximize revenue and minimize delays, healthcare organizations should:
Maintain accurate patient records and insurance information.
Train staff regularly on coding and billing updates.
Monitor key performance indicators (KPIs) like days in accounts receivable, denial rates, and net collection rates.
Adopt technology to automate repetitive tasks.
Engage patients in understanding their financial responsibility upfront.
Healthcare is evolving rapidly, and RCM is no exception. Emerging trends include:
Predictive Analytics – Using historical data to forecast claim denials and optimize cash flow.
Blockchain – Increasingly explored for secure, transparent transactions and patient data sharing.
Patient-Centric Billing – Greater emphasis on providing clear, understandable bills to improve patient satisfaction.
Integration of Telehealth Services – Requires adapting billing processes for virtual care reimbursement.
Revenue Cycle Management (RCM) is not only about finances; it directly affects how patients experience a healthcare organization.
The patient’s financial journey begins at appointment scheduling and registration, not after treatment.
When insurance and personal details are collected accurately, billing errors are significantly reduced.
Patients feel more confident and less stressed when they know what to expect financially before receiving care.
Poor revenue cycle practices, such as incorrect billing or delayed claims, can lead to frustration, confusion, and loss of trust.
Clear communication about:
Co-pays
Deductibles
Insurance coverage
Out-of-pocket costs
helps patients better understand their financial responsibilities.
When patients understand their bills, they are more likely to pay on time.
A well-managed revenue cycle reduces disputes and customer service calls.
Digital billing systems and patient portals allow patients to:
View statements
Track payments
Ask billing questions
Pay online
These tools make the billing process more convenient and improve satisfaction.
Healthcare costs are increasingly being shared by patients, making financial clarity more important than ever.
Providing cost estimates before services are delivered helps patients:
Make informed decisions
Avoid surprise bills
Plan their payments
Transparent billing improves trust between patients and healthcare providers.
When charges are explained in simple terms, patients feel more comfortable paying their bills.
Offering flexible payment plans reduces unpaid balances and improves collections.
Clear, easy-to-read statements prevent confusion and billing disputes.
A transparent revenue cycle benefits:
Patients, by reducing stress and uncertainty
Providers, by improving cash flow
Payers, by reducing claim errors
An efficient and patient-friendly revenue cycle creates a smoother, more reliable healthcare financial system for everyone involved.
The revenue cycle is the lifeblood of any healthcare organization. From patient registration to reimbursement, every stage impacts cash flow, operational efficiency, and patient satisfaction. By understanding each step, addressing challenges, and leveraging modern technology, healthcare providers can optimize revenue collection while focusing on what matters most—quality patient care.
Don’t let compliance delays hinder the growth of your practice.
At Code Credentia, we recognize how prompt licensing and credentialing are vital to your success. Our experts are here to support you every step of the way in:
Delivering accuracy
Efficiency
Peace of mind
Whether you’re just beginning the application process or navigating complex regulatory requirements, we’re here to help.
👉 Request a Free Consultation
📧 Email: info@codecredentia.com
📞 Call: (+1)631-482-7629
Follow us:
Multi-level quality checks ensure flawless Census Entry every time.
We follow strict HIPAA guidelines with secure data handling protocols.
Clean demographic data leads to quicker claim acceptance and payments.
Easily scale Census Entry services as your patient volume grows without hiring overhead.
Our trained professionals understand payer rules, EMR systems, and compliance standards.